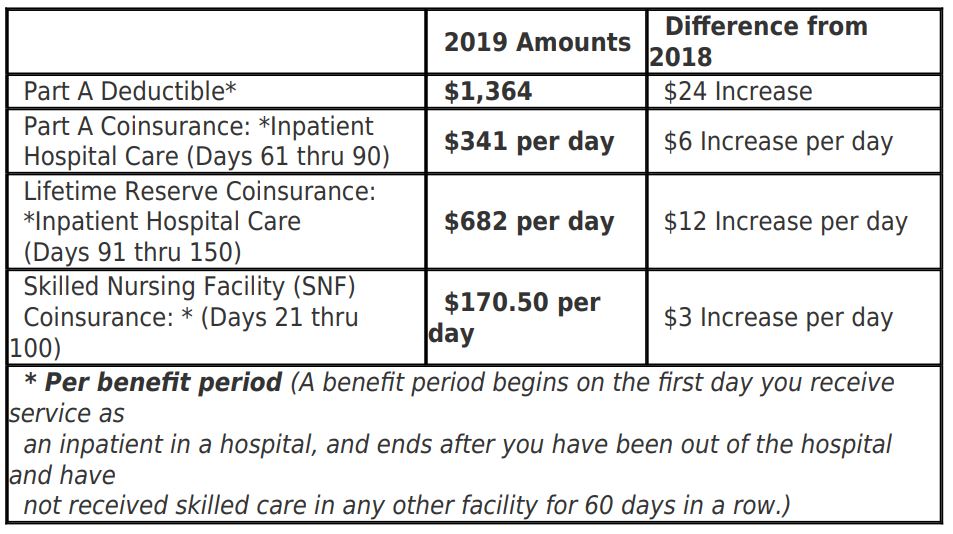
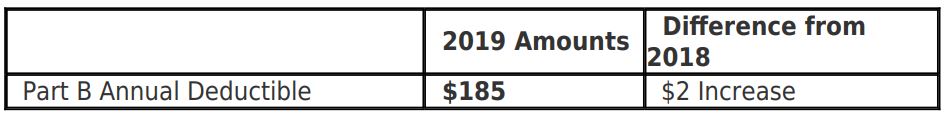
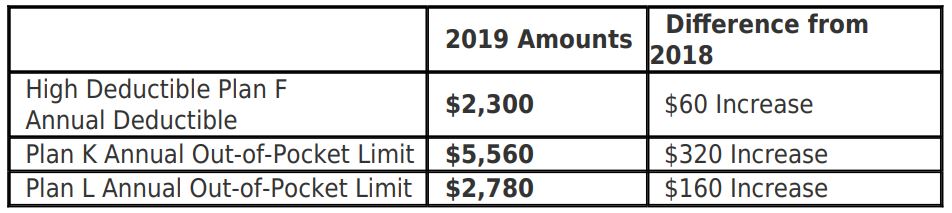
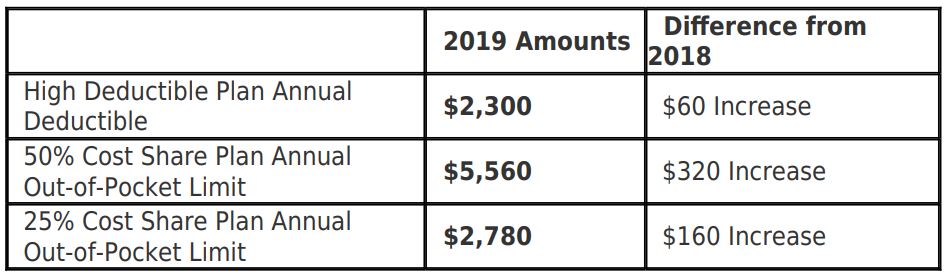
MANY BUSINESS owners don’t think twice when asking a worker to run to the office supply store, to the bank or run another errand for the company while on the clock.
But as soon as that employee enters their personal vehicle on a trip for your business, you automatically become vicariously liable for their actions.
Think it’s not a big deal? There have been cases when employers have been found liable and ordered to pay up to $25 million for crashes involving employees using their cell phones while driving, according to the National Safety Council.
That means if your employee is in an accident and injures a third party, damages another car or injures themselves, your firm could be held liable.
For injuries to only your employee, your workers’ compensation insurance would handle the costs, but for injuries to others and third party property, you are ultimately liable since they were carrying out duties for your firm.
The employee’s auto insurance will be primary, but the problem arises when the coverage is insufficient. The employer can then be sued by the third party.
And once a third party knows there is an employer behind the person who hit them, that often encourages them to sue, seeking, even more, damages than they normally would.
With that in mind, you should do all you can to reduce your exposure by writing a policy for your driving employees (see box on right). Besides having a driving policy in place, you can also make sure to hire employees who are safe drivers by checking their driving records
during the hiring process.
Also, make sure that your management is on board with the policy. That means that managers should avoid texting or calling employees while they are driving on company duty. That would clash with your policy on barring cell-phone use while driving.
Finally, you should make sure that you have proper insurance in place in case calamity strikes. And unfortunately, some employees will inevitably be slack in following even the best laid out policies.
Commercial auto will cover all of your workers who drive company vehicles for collisions, but it won’t cover employees if they are driving their own vehicles while on the job. Such vehicles are considered non-owned autos because they are not owned by the named insured.
Employees are not insureds while driving non-owned autos,
even if they are using the vehicles for company business.
But if you do have workers who use their personal vehicles for
work, like sales reps, you can purchase an endorsement for your commercial auto policy: Entitled Employees as Insureds.
This endorsement covers workers who drive their personal vehicles on behalf of their employer. But it provides excess coverage only, meaning that the employee’s personal auto policy will apply first if the worker is sued after an accident
involving their personal auto. The endorsement would apply only if the employee’s personal policy limits are breached.
ACA Penalties 2018

On November 2, 2017 the Internal Revenue Service (IRS) issued revised FAQs on the employer shared responsibility
provisions under the Affordable Care Act (ACA). Question sets 55-58 now detail the procedure the IRS will use to begin issuing proposed penalty assessments to employers that failed to comply with these provisions in 2015.
Though the IRS was previously silent on the details of penalty assessments, this new information serves as a reminder to employers that compliance enforcement is a priority for the IRS.
Employer Shared Responsibility Provisions
Under the ACA’s employer shared responsibility provisions, Applicable Large Employers (ALEs) are required to o*er health coverage to full-time employees and their dependents that both provides minimum value and is a*ordable. Penalties may be assessed against an
employer that either fails to o*er health coverage to enough of its full-time employees and dependents, or o*ers coverage that fails to provide minimum value and/or meet affordability standards.
In 2015, ALEs were required to o*er coverage to at least 70% of its full-time employees and dependents, and the monthly cost to the employee for self-only coverage could not exceed 9.56% of the employee’s income. ALEs with fewer than 100 full-time employees had transition relief available.
Penalty Assessment Process
The IRS will use Letter 226J to notify employers that it determines, for at least one month of the year, had a full-time employee enrolled in a health plan for which a premium tax credit was allowed. The Letter will include an estimated monthly penalty amount along with a list of full-time employees for whom the penalty applies. Information provided by the employer on 2015 ACA reporting Forms 1094-and 1095-C will be used by the IRS to make these determinations. The IRS intends to issue Letters 226J for the 2015 year in late 2017.
An employer that receives a Letter 226J will have an opportunity to respond to the IRS in writing to either agree with or dispute the IRS’s proposed assessment. In the event a penalty is ultimately assessed, the employer will receive Notice CP220J and will need to
make its payment pursuant to the instructions included therein.
Action Items
While it’s too late for employers to enact compliance strategies that could prevent a 2015 penalty assessment, there are several important considerations for employers going forward:
- If a Letter 226J is received, employers have 30 days to respond to the IRS, in writing, that the employer either agrees with the assessment or disagrees, in whole or in part. Failure to timely respond will result in an automatic assessment of the IRS’s proposed penalty amount.
- Employers should designate a contact person within the organization to handle responses to the IRS should a Letter be received. Accurate record-keeping will be essential, both for past and future years.
- The IRS now has a process through which to administer penalties. Thus, employers should take seriously their ongoing obligations under the ACA, including 2017 ACA reporting.
In an effort to make health coverage more a*ordable and accessible, the Affordable Care Act (ACA) implemented parameters to the premium rating methodologies used by insurers in the individual and small group markets. Insurers in these markets can vary premium based on
age so long as the insurers adhere to the proper age band rating procedure.
This procedure has remained unchanged since 2014, but pursuant to a rule issued by the Department of Health and Human Services (HHS), the rating methodology will change come 2018.
Change to Rating Methodology
Changes to the age band rating methodology will begin to take effect in 2018. Presently, the methodology requires that insurers assign a single banded premium rate for all individuals ages 0-20, with single ratings applied to each year of age from 21 upward (to age 63). Under the new methodology e*ective in 2018, insurers can apply a single banded premium rate for all individuals ages 0-14 and begin to assign a single rate to each year of age as early as age 15. As a result, insureds will begin to see a premium increase upon turning age 15 rather than age 21.
Impact on Employers
Employers in the small group insurance market will be affected by this rating change. In most states, a small group employer is one with 50 or fewer employees. However, California deBnes a small group employer as one with up to 100 full-time and full-time equivalent employees. Thus, a wider swath of employers in California will be impacted than in other states. The new rating methodology will likely bring a premium increase for 2018 renewals for most small group employers. While employers can do little to change their classification as a small group employer and, consequently, the age band ratings that apply, there may be other plan design strategies that could counteract the rising premium costs. Employers should carefully review premium increases expected in 2018 and explore cost-control measures in other areas of their plan.
The state of health insurance: group plans and individual

After months of failed efforts by Congressional Republicans to eliminate the Affordable Care Act, President Trump in October stepped in with two sweeping changes that are reverberating throughout the health insurance system.
The main order he issued immediately eliminates subsidies that are paid to health insurers that participate in government-run exchanges to reduce deductibles and copays for lower-income customers buying individual and family policies.
While some pundits say the move will create chaos in the individual market, they differ on the likely fallout for group policies.
But Trump did sign two other orders that could have a direct effect on the group market over time, but not immediately:
- One would attempt to expand the use of health reimbursement accounts (HRAs), which employers could pay into so that employees can use those funds to purchase health coverage on the open market.
- The other would allow employers to band together to create “association” plans, which would offer plans that are not as comprehensive as dictated by the ACA.
Cost-sharing fallout
Nineteen states have already sued to challenge the cost-sharing reduction subsidies, saying the ACA does not appropriate funding for the subsidies and hence they are illegal. Without them, insurers will likely have to significantly increase their premiums or pull out of the health insurance exchanges.
While the order means many people purchasing plans on the individual market will see drastic rate hikes, the order doesn’t directly affect group plans.
The American Benefits Council, a national trade association based in Washington, D.C. that advocates for employer-sponsored benefit plans, said that the move to cut off the subsidies could spur some insurers to increase their fees for large employer plans in order to make up for the lost revenue in the individual market.
“Employers rely on a healthy and viable individual health insurance marketplace since an unstable market could result in further cost-shifting from health-care providers to large employer plans,” the council said in a prepared statement.
“Additionally, erosion of the ACA exchanges would make individual market coverage a less viable option for part-time workers, early retirees, and those who would otherwise elect to secure coverage through the individual market rather than sign up for, or remain on, COBRA,” it added.
But that sentiment is not universal.